Manual therapy encompasses diverse techniques – soft tissue mobilization, joint mobilization, muscle energy, and neuromuscular approaches – aiming to restore optimal function.
What is Manual Therapy?
Manual therapy is a specialized healthcare practice involving skilled hand techniques to diagnose and treat musculoskeletal pain and dysfunction. Practitioners utilize a comprehensive examination to pinpoint impairments in joints, soft tissues, and the nervous system.
These techniques include myofascial release, addressing restrictions in the connective tissues, and soft tissue mobilization, improving tissue extensibility. Joint mobilization restores optimal joint mechanics, ranging from gentle oscillations to specific adjustments. Muscle energy techniques (MET) leverage patient muscle contractions to correct imbalances.
Furthermore, neuromuscular techniques like proprioceptive neuromuscular facilitation (PNF) enhance movement patterns. Manual therapy isn’t a standalone treatment; it’s often integrated with exercise and other modalities for comprehensive care.
Historical Overview of Manual Therapy
Manual therapy’s roots trace back to ancient civilizations, with early forms of massage and bone-setting documented in Chinese and Greek practices. However, the modern foundations emerged in the late 19th century.
Osteopathy, founded by Andrew Taylor Still in 1874, emphasized the musculoskeletal system’s role in overall health and utilized hands-on techniques. Simultaneously, European practitioners developed various manual approaches. The early 20th century saw the rise of chiropractic, focusing on spinal manipulation.
Throughout the decades, manual therapy evolved, incorporating advancements in anatomy, physiology, and biomechanics. Techniques like myofascial release and muscle energy techniques gained prominence. Today, it’s a globally recognized field, continually refined through research and clinical experience.

Soft Tissue Techniques
Soft tissue techniques address muscles, fascia, and connective tissues, including myofascial release, mobilization, trigger point therapy, and instrument-assisted methods.
Myofascial Release
Myofascial Release (MFR) is a manual therapy technique focused on releasing tension within the myofascial system – the interconnected web of fascia surrounding muscles. Therapists apply sustained pressure into myofascial restrictions to eliminate pain and restore motion.
This technique addresses the restrictions that limit range of motion, contribute to pain, and affect posture. MFR isn’t about forceful stretching; it’s a gentle, sustained approach allowing the fascia to lengthen. It maps soft tissue structures rhythmically, targeting areas of tightness or restriction.
MFR can be utilized on various body areas, including the head, cervical spine, and throughout the body, offering a holistic approach to musculoskeletal health. It’s often incorporated into broader manual therapy plans.
Soft Tissue Mobilization
Soft Tissue Mobilization (STM) encompasses a broad range of manual techniques applied to muscles, tendons, ligaments, and fascia. The goal is to break down adhesions, reduce muscle tension, and improve tissue extensibility. STM techniques vary in intensity and depth, adapting to the patient’s needs.
This method involves hands-on techniques like kneading, stripping, and cross-fiber friction. It’s a fundamental component of manual therapy, often used to address pain, improve range of motion, and enhance overall function. STM is organized by mapping soft tissue structures.
Instrument-Assisted Soft Tissue Mobilization (IASTM) is a specialized form utilizing tools to enhance the effectiveness of STM. It’s a versatile technique integrated into comprehensive treatment plans.
Trigger Point Therapy
Trigger Point Therapy focuses on identifying and releasing hyperirritable spots within skeletal muscle, known as trigger points. These points can cause localized pain or referred pain to other areas of the body. Manual pressure is applied to these points to elicit a release, reducing muscle tension and pain.
Techniques involve sustained pressure, ischemic compression, and stripping to deactivate trigger points. This therapy aims to restore normal muscle function and alleviate pain patterns. It’s often used in conjunction with other soft tissue techniques.
Effective trigger point release can improve range of motion and reduce muscle spasms, contributing to overall pain management and functional restoration. It’s a common component of manual therapy protocols.
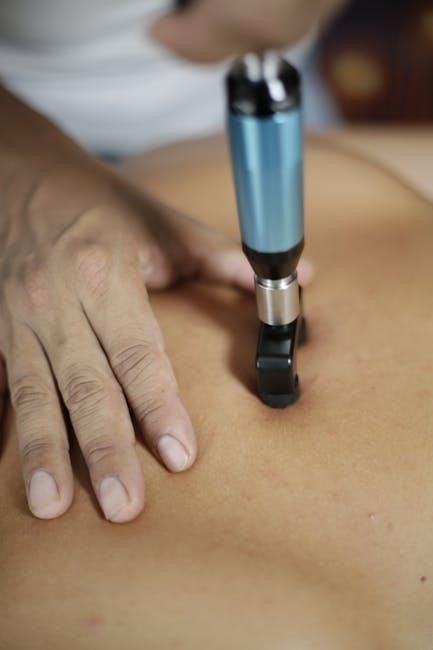
Instrument-Assisted Soft Tissue Mobilization (IASTM)
Instrument-Assisted Soft Tissue Mobilization (IASTM) utilizes specialized tools to detect and treat fascial restrictions and soft tissue dysfunction. These tools, often made of stainless steel, are used to glide over the skin, breaking down adhesions and scar tissue.
IASTM enhances the practitioner’s ability to locate areas of tissue restriction and deliver a focused treatment. It’s effective in addressing conditions like tendinopathies, muscle strains, and scar tissue limitations. The technique aims to restore optimal tissue mobility and reduce pain.
By applying controlled pressure, IASTM promotes increased blood flow and improved tissue healing. It’s frequently integrated with other manual therapy approaches for comprehensive care.
Joint Mobilization Techniques
Joint mobilization involves skilled hand movements to restore joint mechanics, reduce pain, and improve range of motion through graded oscillations.
Grade I Mobilization
Grade I mobilization represents a very gentle technique, primarily focused on assessing joint play rather than creating significant joint movement. Therapists apply small-amplitude, rhythmic oscillations near the beginning of the available range of motion.
The primary goal isn’t to stretch capsules or ligaments, but to detect subtle restrictions and provide a soothing, pain-relieving effect. Patients often describe a comfortable, rhythmic sensation. This grade is frequently used in acute inflammation or when pain significantly limits movement. It’s characterized by a “take-up” of slack, meaning the therapist feels for any resistance or restriction as they gently move the joint.
It’s a crucial initial step in evaluating and addressing joint dysfunction, establishing a baseline for further treatment progression.
Grade II Mobilization
Grade II mobilization involves slightly larger amplitude oscillations than Grade I, still within the available range of motion, but moving further into it. The therapist aims to access and treat joint restrictions, initiating a therapeutic stretch to the joint capsule and surrounding ligaments.
This technique is often used to address joint stiffness and improve range of motion in subacute conditions. Patients typically feel a gentle stretching sensation, and the therapist can perceive a definite resistance followed by a slight give as the restriction is addressed.
Grade II mobilizations are rhythmic and repetitive, promoting viscoelastic changes within the joint tissues, ultimately enhancing joint mobility and reducing pain.
Grade III Mobilization
Grade III mobilization utilizes a larger amplitude, rhythmic oscillatory movement, reaching the limit of the available range of motion. Unlike Grade II, it aims to directly address joint restrictions by overcoming them, inducing a stretch to the capsule and ligaments.
Patients will experience a more noticeable stretch sensation, and the therapist will feel a clear resistance that momentarily “breaks” as the restriction yields. This technique is frequently employed for joints exhibiting moderate restrictions and is often used to restore full range of motion.
Grade III mobilizations are performed rhythmically, promoting significant viscoelastic changes and reducing joint stiffness, contributing to pain reduction and improved function.
Grade IV Mobilization
Grade IV mobilization represents a high-amplitude oscillatory technique performed at the end range of motion. It’s characterized by a sustained stretch applied to the joint capsule and surrounding tissues, aiming to disrupt adhesions and restore optimal joint mechanics.
The therapist will feel a distinct “stretch” and a firm resistance, maintaining the force until a noticeable change occurs in joint play. Patients may experience some discomfort, but it should remain within tolerable limits. This grade is reserved for joints with significant restrictions.
Grade IV mobilizations are carefully applied, focusing on restoring joint play and reducing pain by addressing capsular restrictions and improving overall joint mobility.
High-Velocity, Low-Amplitude (HVLA) Thrust Techniques
HVLA thrust techniques, often referred to as “adjustments,” involve a rapid, small-amplitude force applied to a specific joint. This technique aims to restore joint play by overcoming restrictive patterns and momentarily separating joint surfaces.
A characteristic “cavitation” sound – a popping noise – may be heard or felt during an HVLA thrust, indicating gas release within the joint capsule. While not essential for effectiveness, it’s a common occurrence.
HVLA is typically used for joints exhibiting hypomobility, and requires precise patient positioning and skilled application to ensure safety and efficacy. Careful screening for contraindications is crucial before performing this technique.

Muscle Energy Techniques (MET)
Muscle Energy Techniques utilize gentle muscular contractions by the patient, against a precisely controlled counterforce from the therapist, to restore joint motion.
Postisometric Relaxation (PIR)
Postisometric Relaxation (PIR) is a core Muscle Energy Technique (MET) involving a brief, gentle isometric contraction of the targeted muscle. This contraction is held for a specified duration – typically 5-10 seconds – against an opposing force provided by the therapist.
Following the isometric contraction, the patient is instructed to completely relax the muscle. During this relaxation phase, the therapist gently moves the joint through a newly gained range of motion. The principle behind PIR is that the isometric contraction temporarily increases muscle excitability, followed by a reciprocal inhibition of the antagonist muscles during the relaxation phase.
This allows for a more effective stretch and lengthening of the shortened muscle, ultimately improving joint mobility and reducing muscle tension. PIR is frequently employed to address muscle imbalances and restrictions in various joints throughout the body.
Reciprocal Inhibition (RI)
Reciprocal Inhibition (RI), another vital Muscle Energy Technique (MET), leverages the neurological principle where contraction of a muscle group automatically causes relaxation in its opposing muscle group. The therapist applies a gentle force to activate the antagonist muscle, intending to inhibit the overactive agonist.
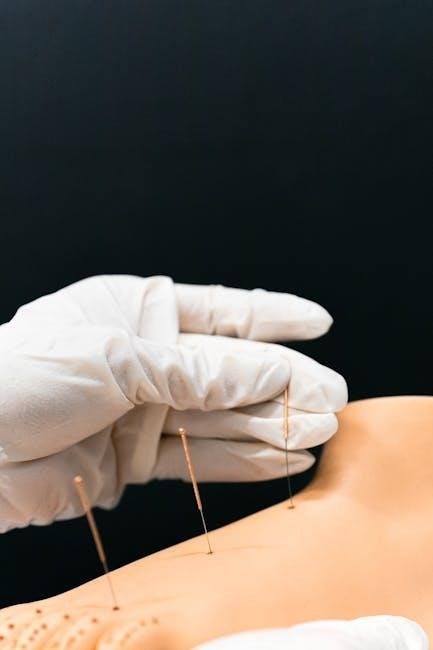
Unlike PIR, RI doesn’t typically involve a sustained isometric contraction of the restricted muscle itself. Instead, the focus is on stimulating the opposing muscle to facilitate relaxation of the tight muscle. The patient is encouraged to assist with the movement, but without actively contracting the restricted muscle.
This technique is particularly useful when a muscle is guarded or difficult to stretch directly. By utilizing the nervous system’s natural inhibitory mechanisms, RI can effectively reduce muscle spasm and improve range of motion, restoring balanced muscle function.
Active Assisted Techniques
Active Assisted Techniques represent a core component of Muscle Energy Techniques (MET), bridging the gap between passive and active movements. Here, the patient contributes to the movement as much as they are able, while the therapist provides a gentle assisting force to guide and enhance the range of motion.
This approach is particularly beneficial when a patient has limited strength or control, or when attempting to overcome a muscle’s guarding response. The therapist carefully monitors the patient’s response, ensuring the force applied is appropriate and doesn’t cause pain.
Active assistance encourages neuromuscular re-education, promoting improved muscle activation and coordination. It’s a versatile technique applicable to various joint restrictions and muscle imbalances, fostering patient participation and promoting functional recovery.
Neuromuscular Techniques
Neuromuscular Techniques, like Proprioceptive Neuromuscular Facilitation (PNF) and Strain-Counterstrain, focus on modulating nervous system input to reduce muscle tension and pain.
Proprioceptive Neuromuscular Facilitation (PNF)
Proprioceptive Neuromuscular Facilitation (PNF) is a sophisticated manual therapy approach that leverages the body’s natural neuromuscular mechanisms to enhance or inhibit muscle activity. It utilizes specific patterns of muscle contraction and relaxation, often involving diagonal movement patterns, to improve range of motion and reduce muscle spasms.
PNF techniques commonly involve a combination of stretching and resisted contractions. Key principles include utilizing the patient’s own muscle efforts, providing tactile cues, and incorporating rhythmic stabilization. Different PNF techniques exist, such as hold-relax, contract-relax, and hold-relax with agonist contraction, each designed to target specific neuromuscular responses.
This method is frequently employed to address muscle tightness, improve joint mobility, and restore functional movement patterns, making it a valuable tool in rehabilitation and pain management.
Strain-Counterstrain
Strain-Counterstrain is a gentle, patient-centered manual therapy technique founded on the principle that tender points indicate areas of acute muscular strain and associated pain. The technique aims to alleviate pain by passively positioning the patient into a “position of comfort” that shortens the affected muscle.
This comfortable position is held for a specific duration, typically 90 seconds, allowing the nervous system to reset and reduce the strain on the tender point. Unlike forceful manipulations, Strain-Counterstrain relies on finding positions that reduce discomfort, rather than pushing through it.
It’s a highly effective method for addressing a wide range of musculoskeletal conditions, particularly those involving chronic pain and muscle spasms, offering a non-invasive and well-tolerated treatment option.

Specialized Manual Therapy Approaches
Specialized techniques, like visceral manipulation, cranial osteopathy, and lymphatic drainage, address unique systems for holistic healing and improved body function.
Visceral Manipulation
Visceral Manipulation (VM) is a gentle, hands-on therapy focused on the diagnosis and treatment of the deep fascial restrictions within the body’s internal organs – the viscera. This specialized approach recognizes that these organs can become restricted due to surgery, trauma, infection, or even habitual posture.
The goal of VM isn’t to directly manipulate the organs themselves, but rather to release the restrictions in the surrounding connective tissues. By restoring the natural mobility and relationship of the viscera, VM aims to improve musculoskeletal function, reduce pain, and enhance overall health. Practitioners use subtle, rhythmic movements to encourage the body’s self-corrective abilities.
VM can address a wide range of conditions, including digestive issues, chronic pain, and postural imbalances, by restoring optimal visceral function and promoting a more balanced state within the body.
Cranial Osteopathy
Cranial Osteopathy is a refined and subtle branch of osteopathic treatment, focusing on the craniosacral system – comprised of the skull, the membranes and fluid surrounding the brain and spinal cord, and the sacrum. It operates on the principle that this system exhibits a subtle, inherent rhythm, and restrictions within it can contribute to a variety of health issues.
Practitioners use extremely gentle, hands-on techniques to detect and release restrictions in this system, encouraging the natural mobility and balance of the craniosacral rhythm. These techniques involve very light pressure and are often described as a “palpable tide.”
Cranial Osteopathy is used to address conditions like headaches, migraines, TMJ disorders, and even emotional trauma, by restoring optimal function and promoting the body’s self-healing capabilities.
Lymphatic Drainage Therapy
Lymphatic Drainage Therapy (LDT), also known as manual lymphatic drainage, is a gentle technique designed to encourage the natural drainage of the lymph, which is part of the body’s immune system. It aims to facilitate the removal of waste and toxins from bodily tissues, reducing swelling and supporting immune function.
LDT utilizes light, rhythmic strokes applied in a specific sequence to stimulate lymphatic flow. These movements follow the direction of the lymphatic vessels, guiding fluid towards lymph nodes where it can be filtered.
This therapy is often used to address lymphedema, post-surgical swelling, and chronic venous insufficiency, promoting detoxification and overall wellness through improved lymphatic circulation.
Manual Therapy for Specific Conditions
Manual therapy effectively addresses conditions like back pain, neck pain, and headaches, utilizing targeted techniques to alleviate discomfort and restore function.
Manual Therapy for Back Pain
Manual therapy offers a multifaceted approach to managing back pain, employing techniques tailored to the specific source of discomfort. Soft tissue mobilization addresses muscle tension and myofascial restrictions contributing to pain, while joint mobilization restores proper spinal movement and reduces stiffness.
Muscle energy techniques (MET) help re-educate muscles and improve spinal alignment, and neuromuscular techniques like strain-counterstrain aim to alleviate pain by reducing muscle spasms. Furthermore, approaches like myofascial release can address broader connective tissue imbalances.
The integration of these techniques, alongside exercise, provides a comprehensive strategy for pain reduction, improved function, and long-term management of back pain conditions. Careful assessment is crucial to determine the most appropriate manual therapy interventions.
Manual Therapy for Neck Pain
Manual therapy provides targeted interventions for neck pain, addressing both muscular and joint dysfunction. Soft tissue techniques, including myofascial release, alleviate tension in neck and shoulder muscles often contributing to headaches and restricted movement. Joint mobilization, utilizing graded approaches, restores optimal cervical spine mechanics and reduces stiffness.
Muscle energy techniques (MET) can correct postural imbalances and improve neck alignment, while neuromuscular techniques offer pain relief by addressing muscle spasms. Specific techniques focusing on the head and cervical spine are often employed.
Combining these manual approaches with therapeutic exercise enhances long-term stability and function, offering a holistic treatment strategy for neck pain sufferers.
Manual Therapy for Headaches
Manual therapy offers a multifaceted approach to headache management, targeting musculoskeletal contributors to pain. Soft tissue mobilization, particularly myofascial release, addresses tension in the neck, shoulders, and head, frequently implicated in tension-type headaches. Joint mobilization of the cervical spine restores proper movement and reduces nerve irritation.
Muscle energy techniques (MET) can correct postural imbalances that exacerbate headaches, while strain-counterstrain aims to alleviate tender points. Techniques impacting myofascial structures of the head and cervical spine are often utilized.
Integrating manual therapy with exercise and other modalities provides comprehensive headache relief and preventative care.

Integration with Other Therapies
Manual therapy is often enhanced by combining it with exercise, ultrasound, or cryotherapy, creating a synergistic effect for improved patient outcomes.
Manual Therapy and Exercise
Combining manual therapy with exercise represents a cornerstone of effective rehabilitation. Manual techniques address immediate restrictions in joint mobility or soft tissue flexibility, preparing the body for active movement patterns. Exercise then reinforces these gains, building strength, endurance, and functional stability.
This integrated approach isn’t simply sequential; it’s often performed concurrently. For example, a joint mobilization might be immediately followed by specific exercises to retrain neuromuscular control around that joint. Exercise helps prevent recurrence of dysfunction by addressing underlying muscle imbalances and movement impairments. The goal is to empower patients to actively participate in their recovery and maintain long-term improvements, moving beyond passive treatment towards self-management.
Manual Therapy and Ultrasound Therapy
Integrating manual therapy with ultrasound therapy offers a synergistic approach to musculoskeletal care. Manual techniques address mechanical restrictions – joint stiffness or muscle tension – while ultrasound delivers therapeutic energy to deeper tissues. Ultrasound can promote tissue healing, reduce inflammation, and increase blood flow, complementing the biomechanical effects of manual interventions.
Often, manual therapy is applied before ultrasound to optimize tissue extensibility and enhance ultrasound penetration. However, the sequence can be adjusted based on individual needs. Ultrasound’s thermal effects can prepare tissues for more effective manual techniques. This combined modality is frequently utilized for conditions like tendinopathies, muscle strains, and joint capsular restrictions, providing comprehensive treatment addressing both structural and physiological components of pain and dysfunction;
Manual Therapy and Cryotherapy
Combining manual therapy with cryotherapy – the application of cold – provides a powerful strategy for managing acute musculoskeletal injuries and inflammation. Manual techniques, such as soft tissue mobilization or joint mobilization, can address biomechanical impairments, while cryotherapy reduces pain, swelling, and muscle spasm. This dual approach targets both the structural and inflammatory aspects of injury.
Cryotherapy is often applied after manual therapy to minimize post-treatment inflammation and manage any discomfort. However, careful consideration is needed, as cold can temporarily reduce tissue extensibility. Therefore, the timing and duration of cryotherapy must be individualized. This integrated approach is particularly beneficial for acute sprains, strains, and post-surgical rehabilitation, promoting faster recovery and improved functional outcomes.
Contraindications and Precautions
Manual therapy requires careful screening for contraindications like fractures, infections, and systemic diseases; precautions include respecting pain limits and patient comfort.
Absolute Contraindications
Absolute contraindications to manual therapy represent conditions where treatment is unequivocally harmful and should never be performed. These include acute inflammatory arthritis, active infection (local or systemic), acute fractures or dislocations, and bony instability.
Malignancy, particularly if metastatic, is a strict contraindication, as manipulation could spread cancerous cells. Severe osteoporosis with high fracture risk also falls into this category. Furthermore, any acute neurological signs, such as cauda equina syndrome or progressive neurological deficits, necessitate immediate medical referral, precluding manual therapy.
Patients with acute cardiovascular instability, such as recent myocardial infarction or uncontrolled hypertension, should not receive manual treatment. Finally, any condition where palpation or movement exacerbates symptoms significantly constitutes an absolute contraindication, demanding cautious assessment and alternative approaches.
Relative Contraindications
Relative contraindications to manual therapy require careful consideration and individualized assessment before proceeding. These conditions don’t automatically exclude treatment but demand heightened caution and modified techniques. Examples include pregnancy, particularly the first trimester, and significant organ dysfunction like kidney failure or liver disease.
Patients taking anticoagulant medications require careful monitoring due to increased bleeding risk. Similarly, individuals with uncontrolled diabetes or autoimmune diseases necessitate a cautious approach. The presence of psychological distress or cognitive impairment may also warrant modification or deferral of treatment.
Acute muscle spasm or severe pain may be a relative contraindication, requiring initial pain management before manual intervention. Ultimately, the therapist must weigh the potential benefits against the risks, prioritizing patient safety and informed consent.

